
One Year Clinical Trial Outcomes Provide Evidence for Changing the Way We Care for Patients with Type 2 Diabetes

Every day in the U.S., more than 3,800 adults see their physician and learn that they have a new diagnosis—type 2 diabetes. Living with type 2 diabetes can be a burden for many, as it’s often associated with reduced quality of life through social², work³, and economic⁴ challenges.
Virta is changing that.
We combined decades of scientific research to develop a new, patient-centered comprehensive care model to reverse diabetes, rather than just manage it. We provide patients with a technology-enabled remote care team—a health coach and physician who continuously customize care plans for patients, helping them achieve and sustain nutritional ketosis, behavior change, and reach their goals. Patients regularly log biomarkers and subjective feedback via an app, while the remote care team monitors this information to further personalize their care, and physicians adjust medications as needed. Patients are also supported by peers through an online social community. We hypothesized that this care model would improve health for patients with type 2 diabetes, so we put it to the test in a clinical trial.
This trial enrolled 262 adult volunteers with type 2 diabetes who chose to receive this new, continuous care intervention utilizing nutritional ketosis (Virta Treatment). For comparison, the study also enrolled 87 adult volunteers who received the typical care and support for treatment of type 2 diabetes (Usual Care), including appointments with their physician and consultations with registered dietitians regarding nutrition and lifestyle changes recommended by the American Diabetes Association.
Patients receiving the continuous care intervention from Virta had significant reductions in HbA1c, weight, and medication use in 10 weeks.⁵ Rightfully so, many people wondered if these improvements could be sustained for a longer period of time. After one year, this is how the health outcomes for participants enrolled in the trial have changed⁶:
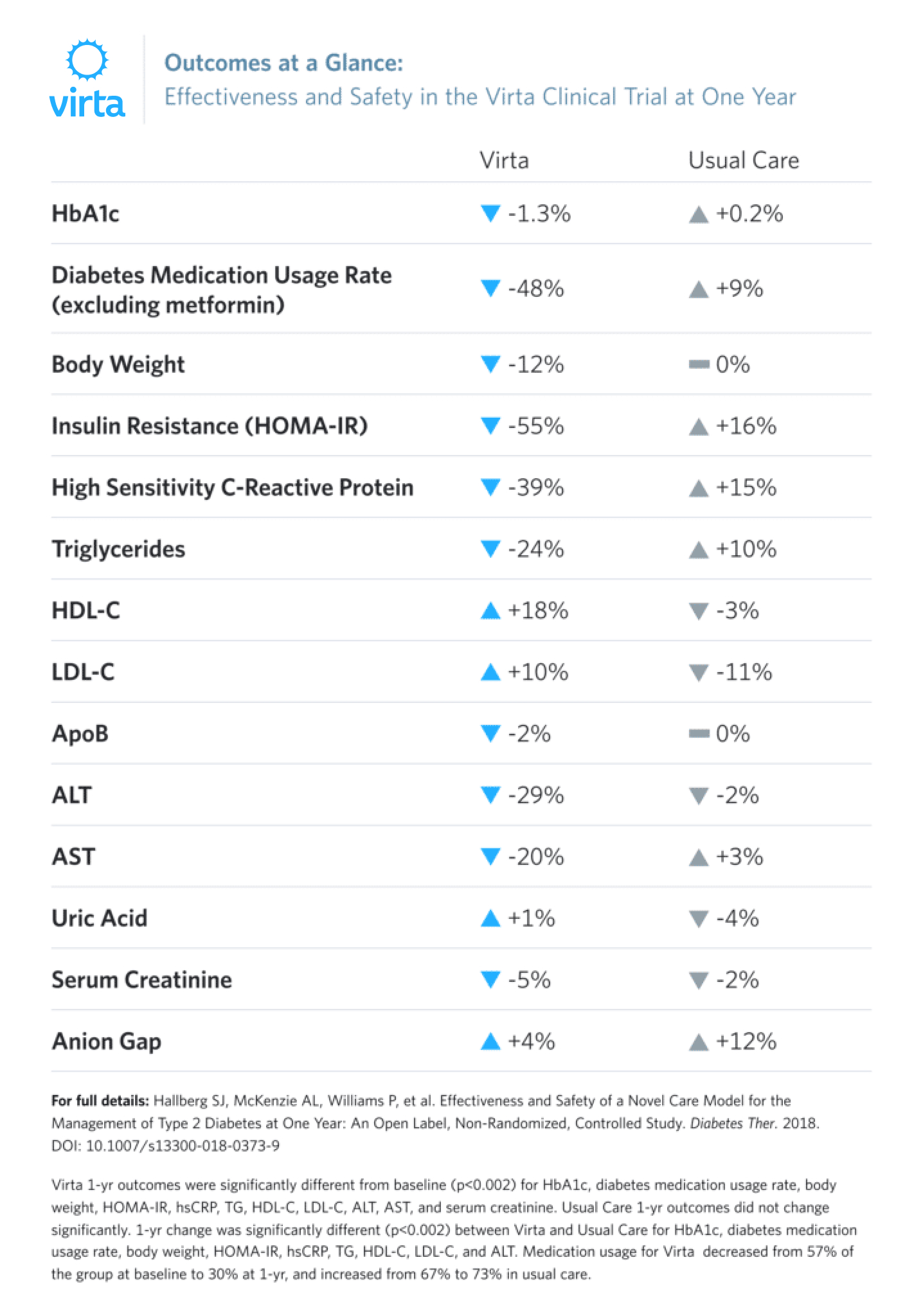
These results demonstrate that there are alternatives to usual care that improve health outcomes in patients with type 2 diabetes. Glycemic control can improve and be sustained while simultaneously reducing or eliminating medications and losing weight. Not only can this intervention be delivered without negative impact on other aspects of health, it also improves atherogenic dyslipidemia, blood pressure, elevated liver enzymes, and inflammation.
How does this change care for type 2 diabetes?
Chronic disease management is often challenged by fractionated care with infrequent follow up visits⁷ and limited physician time.⁸ This intervention changes that. The patient’s remote care team at Virta, supported by software and data, is always there to provide medical care, nutrition advice, accountability, and support.
Management of type 2 diabetes is commonly approached with pharmaceuticals to achieve better glycemic control, but these options are sometimes associated with increased cardiovascular risk⁹ or weight gain.¹⁰ This intervention changes that. Patients can lower HbA1c without increasing cardiovascular risk or weight and while improving multiple independent cardiovascular risk factors.
Lifestyle change is often the first line of defense against the consequences of diabetes and comes with less risk and cost than other treatment options. In trials¹¹,¹², a number of metabolic or lifestyle interventions appear to have similar 1-year outcomes to Virta’s treatment, but these studies sometimes excluded patients with long-standing type 2 diabetes or who were prescribed insulin. This study changes that. The average Virta patient in this trial had diabetes for 8 years and 30% of participants were prescribed insulin when they enrolled; 94% of insulin users were able to reduce or eliminate the medication and 60% of participants were able to reverse their type 2 diabetes at one year.
The outcomes of this clinical trial are promising, but there’s so much more to learn.
Research interest in nutritional ketosis, a physiologically-induced means of safely elevating blood beta-hydroxybutyrate, has skyrocketed in the last few years with studies in both human and animal models and evidence mounting to suggest it has a broad range of health benefits. The research team at Virta is excited to dig into the details of utilizing nutritional ketosis for reversal of type 2 diabetes to further scientific understanding and to better inform clinical care decisions.
It’s clear from these data that improvement in type 2 diabetes can be sustained through one year for the majority of participants receiving treatment from Virta, but one year isn’t a lifetime. We know this lifestyle change to reverse type 2 diabetes requires a long-term commitment from our patients, so we’re committed to our patients by learning more about our care model. To help accomplish this, we extended this clinical trial to 5 years. We couldn’t be more excited about the opportunity we have to learn more about management of chronic disease while continuously improving both the quality of our clinical care and the long-term health outcomes of our patients.
The information we provide at virtahealth.com and blog.virtahealth.com is not medical advice, nor is it intended to replace a consultation with a medical professional. Please inform your physician of any changes you make to your diet or lifestyle and discuss these changes with them. If you have questions or concerns about any medical conditions you may have, please contact your physician.
This blog is intended for informational purposes only and is not meant to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition or any advice relating to your health. View full disclaimer
Are you living with type 2 diabetes, prediabetes, or unwanted weight?

- Centers for Disease Control and Prevention. National Diabetes Statistics Report, 2017. Accessed at: https://www.cdc.gov/diabetes/pdfs/data/statistics/national-diabetes-statistics-report.pdf
- Feng X, Astell-Burt T. Impact of a type 2 diabetes diagnosis on mental health, quality of life, and social contacts: a longitudinal study. BMJ Open Diab Res Care. 2017 Feb 16;5(1):e000198–6.
- Lavigne JE, Phelps CE, Mushlin A, Lednar WM. Reductions in individual work productivity associated with type 2 diabetes mellitus. Pharmacoeconomics. 2003;21(15):1123–34.
- American Diabetes Association. Economic Costs of Diabetes in the U.S. in 2012. Diabetes Care 2013 Apr; 36(4): 1033-1046.
- McKenzie A, Hallberg S, Creighton BC, Volk BM, Link T, Abner M, et al. A Novel Intervention Including Individualized Nutritional Recommendations Reduces Hemoglobin A1c Level, Medication Use, and Weight in Type 2 Diabetes. JMIR Diabetes. 2017;2(1):e5.
- Hallberg SJ, McKenzie AL, Williams P, et al. Effectiveness and Safety of a Novel Care Model for the Management of Type 2 Diabetes at One Year: An Open Label, Non-Randomized, Controlled Study. Diabetes Ther. 2018. DOI: 10.1007/s13300-018-0373-9
- Wagner EH, Austin BT, Davis C, Hindmarsh M, Schaefer J, Bonomi A. Improving Chronic Illness Care: Translating Evidence Into Action. Health Affairs. 2001 Nov 1;20(6):64–78.
- Ostbye T. Is There Time for Management of Patients With Chronic Diseases in Primary Care? The Annals of Family Medicine. 2005 May 1;3(3):209–14.
- The ACCORD Study Group. Long-Term Effects of Intensive Glucose Lowering on Cardiovascular Outcomes. N Engl J Med. 2011 Mar 3;364(9):818–28.
- Henry RR, Gumbiner B, Ditzler T, Wallace P, Lyon R, Glauber HS. Intensive conventional insulin therapy for type II diabetes. Metabolic effects during a 6-mo outpatient trial. Diabetes Care. 1993 Jan;16(1):21–31.
- Lean ME, Leslie WS, Barnes AC, Brosnahan N, Thom G, McCombie L, et al. Primary care-led weight management for remission of type 2 diabetes (DiRECT): an open-label, cluster-randomised trial. Lancet. 2017 Dec 4.
- Saslow LR, Daubenmier JJ, Moskowitz JT, Kim S, Murphy EJ, Phinney SD, et al. Twelve-month outcomes of a randomized trial of a moderate-carbohydrate versus very low-carbohydrate diet in overweight adults with type 2 diabetes mellitus or prediabetes. Nutr Diab. 2017 Dec 8.






.jpg)

