
Decades of research supported by ongoing clinical studies
Clinical outcomes
Type 2 Diabetes
While reducing and eliminating glycemic control medications, Virta patients lowered HbA1c by 1.3% on average after one year and improved insulin resistance measured by HOMA-IR. 60% of patients enrolled one year attained an HbA1c below 6.5% without the use of diabetes medications other than metformin.¹

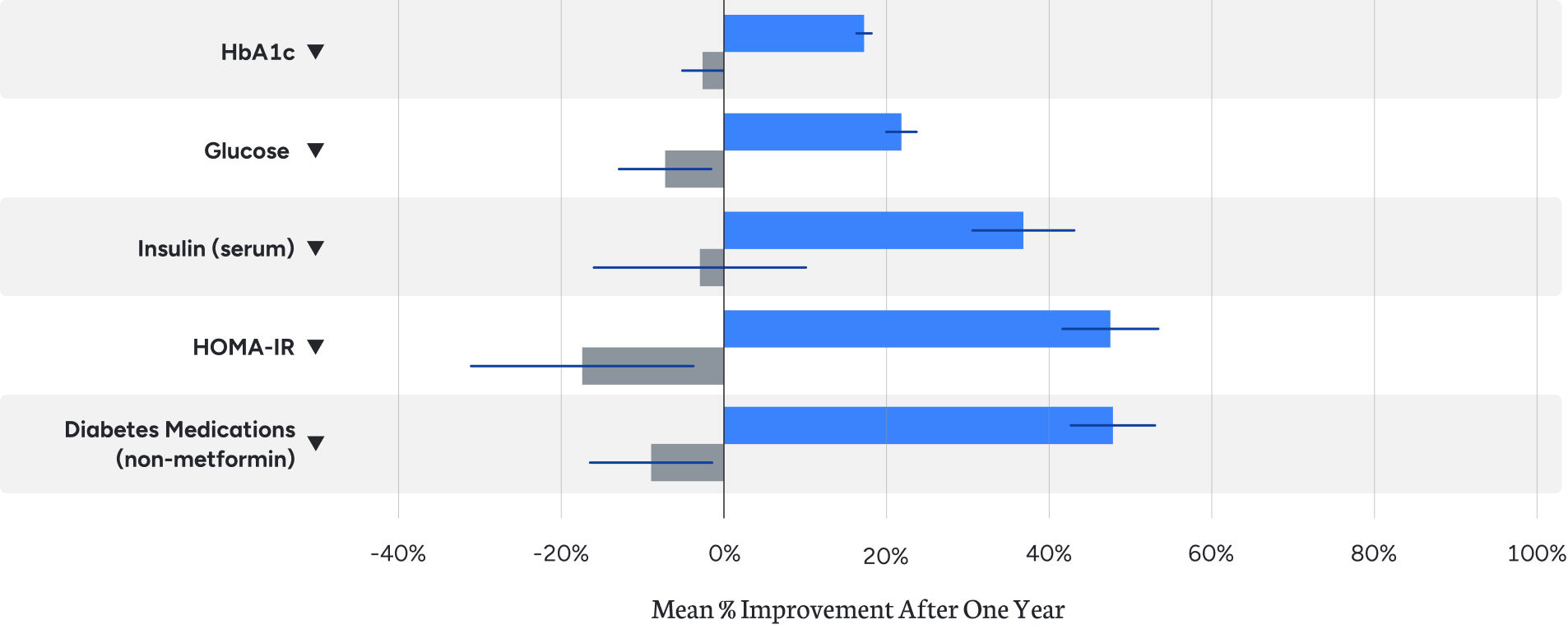
Obesity
Excess weight represents risk for both type 2 diabetes and cardiovascular disease. Virta patients with type 2 diabetes sustained the loss of 12% of their body weight over the year. The prevalence of class III obesity among participants was reduced from 46% to 20%.¹

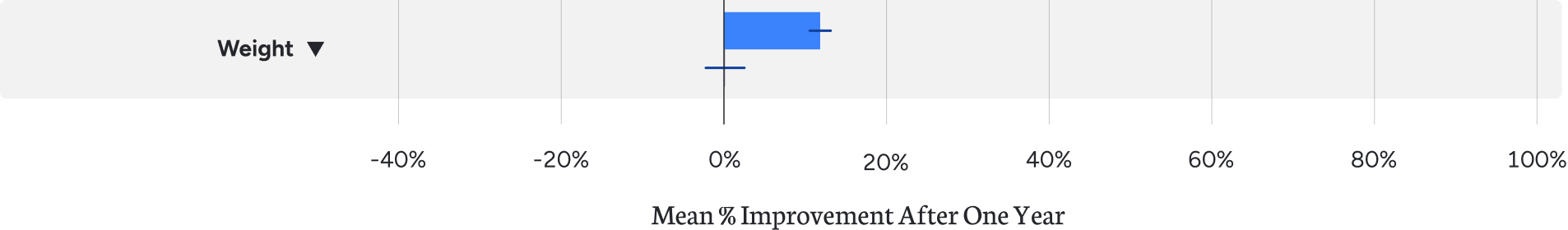
Atherogenic Dyslipidemia
Characterized by high triglycerides and low HDL-C, atherogenic dyslipidemia is common among patients with insulin resistance and represents increased cardiovascular risk. Virta patients improved both markers, with the TG/HDL-C ratio declining from 4.7 to 3 on average.¹

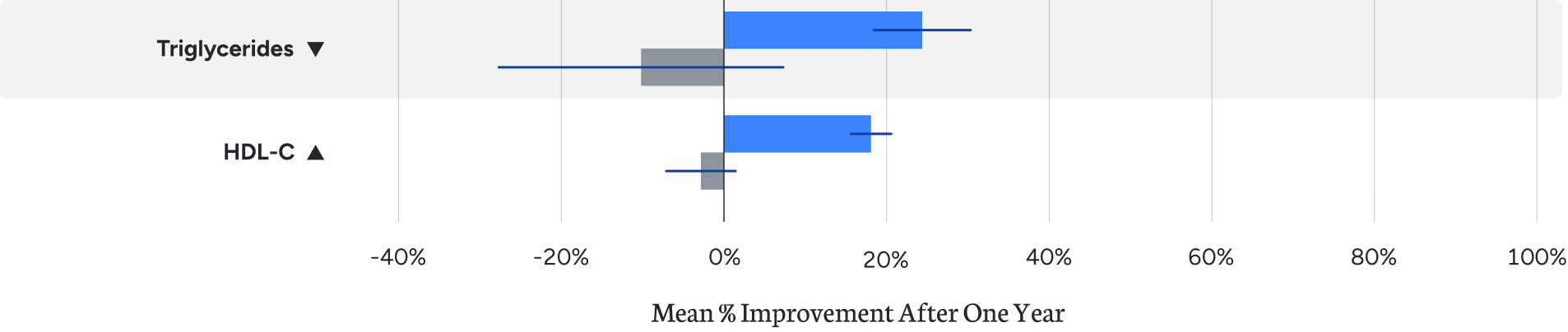
Hypertension
Elevated blood pressure, especially in the presence of additional risk factors, increases cardiovascular risk. Virta patients reduced blood pressure and the need for antihypertensive medication, especially diuretics.¹

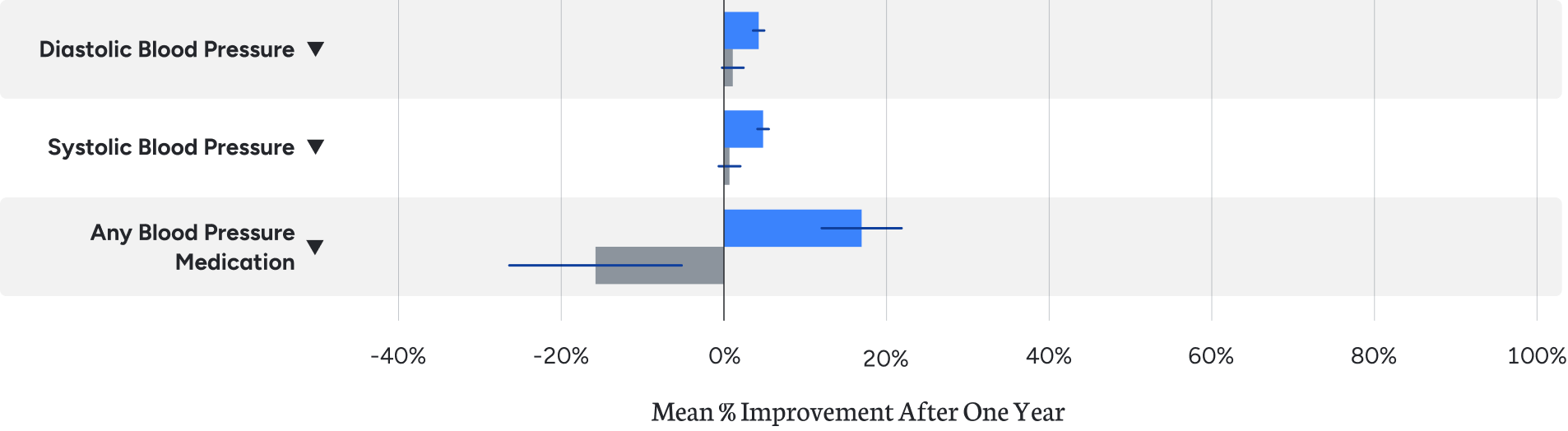
Inflammation
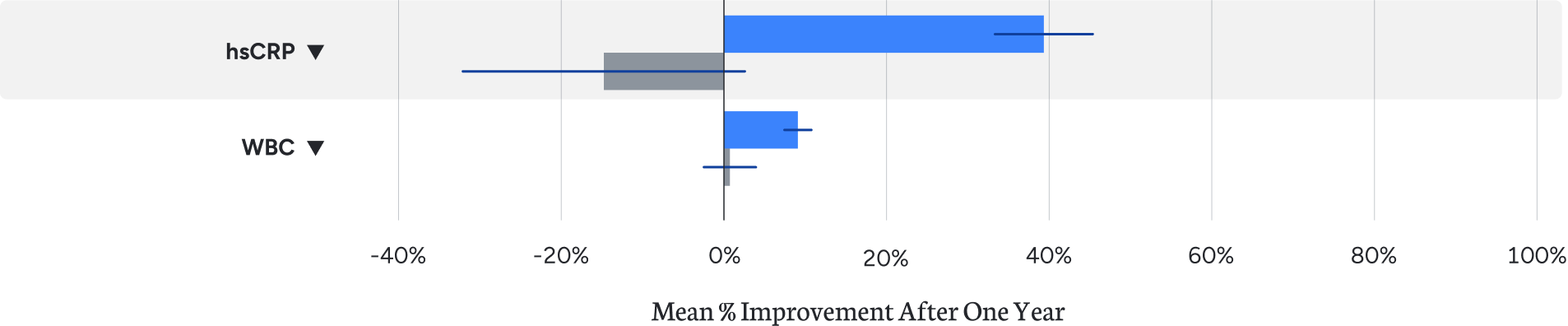
Inflammation is a common underlying factor in obesity, insulin resistance, hypertension, and cardiovascular disease. C-reactive protein and white blood cell count, common markers of inflammation, were significantly reduced in Virta patients with type 2 diabetes.¹

Safety
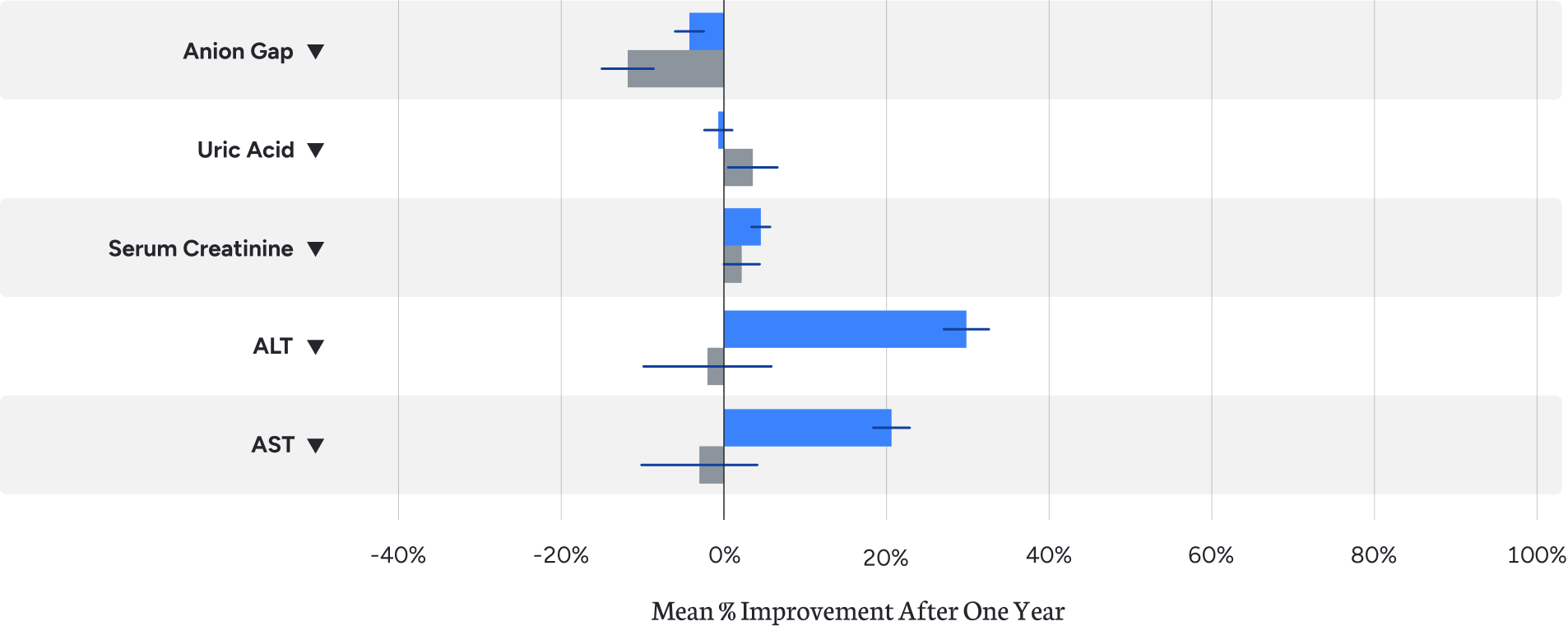
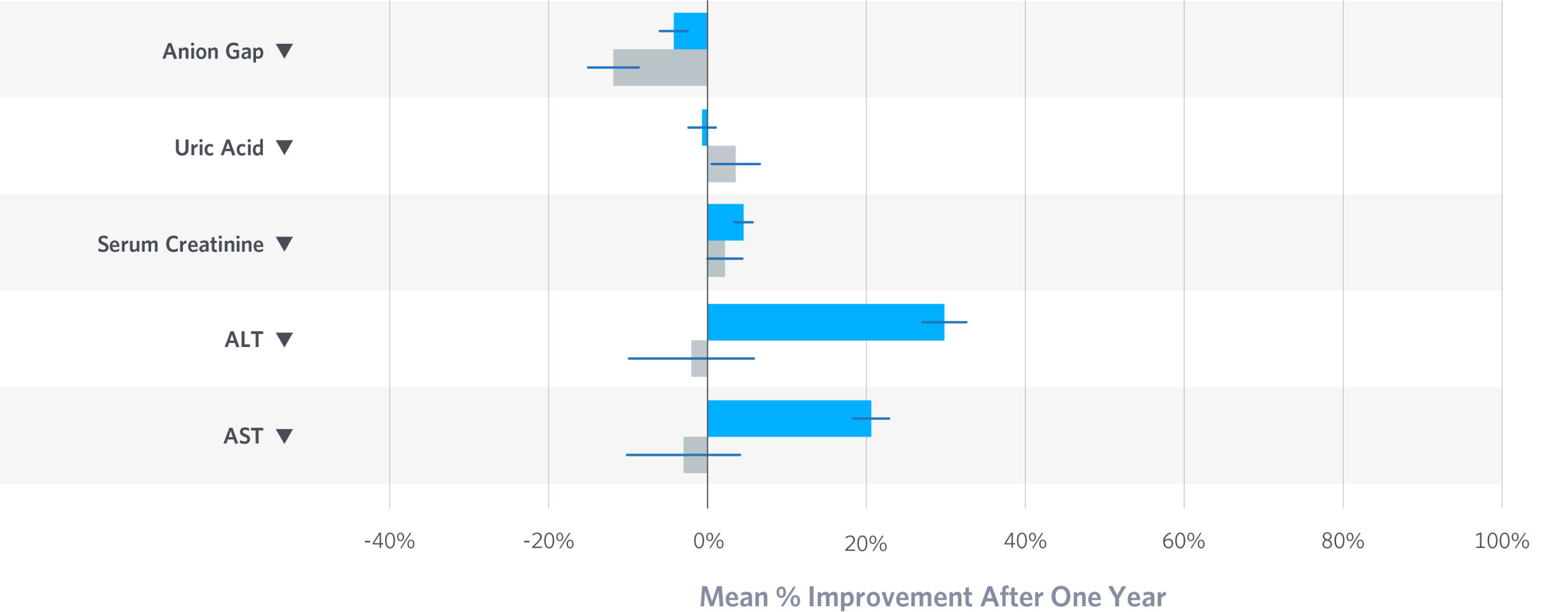
A common concern in the treatment of type 2 diabetes is hypoglycemia. In our clinical trial, no hypoglycemic events requiring assistance were reported. Additionally, treatment at Virta resulted in neutral or positive effects on markers of kidney and liver function.¹

Cardiovascular Risk Measures
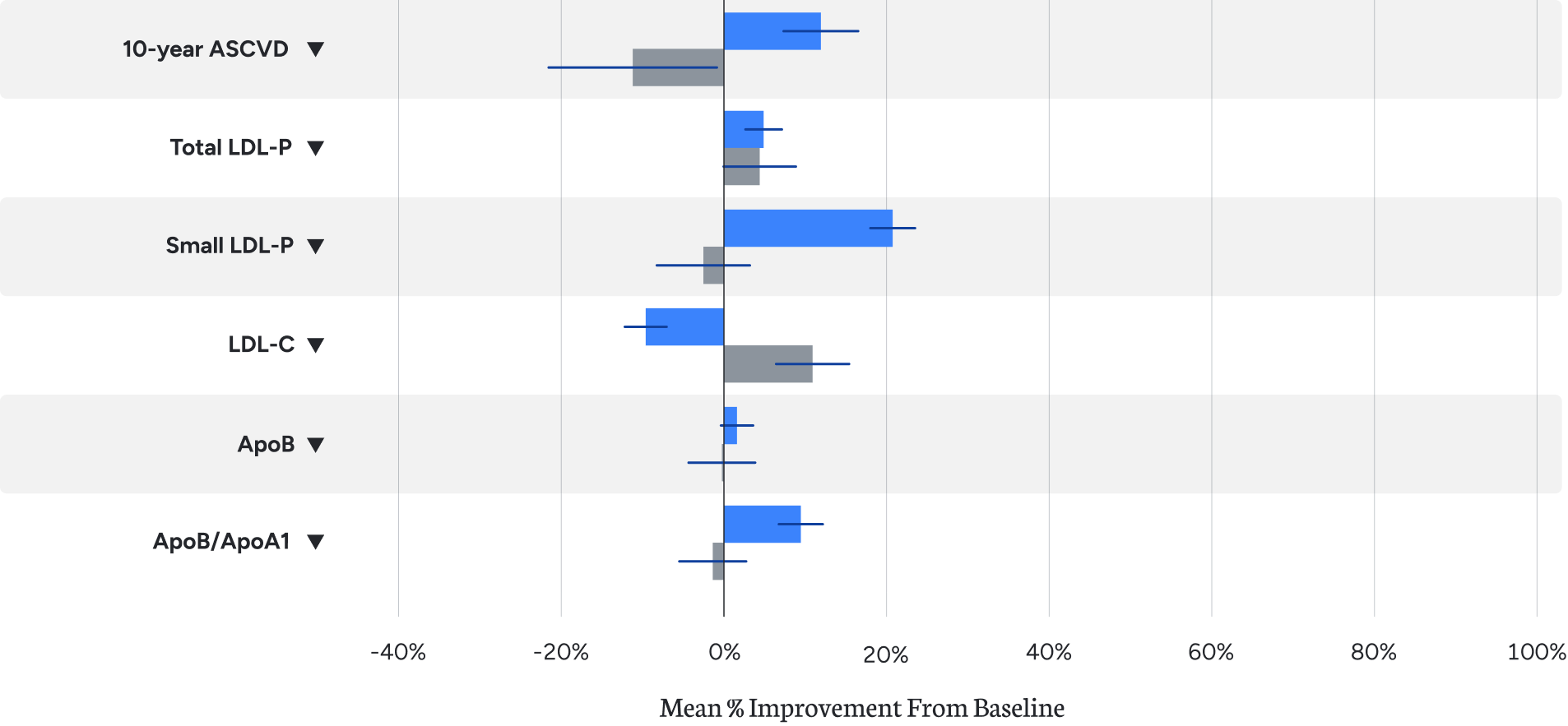
10-year ASCVD risk score improves after one year of the Virta Treatment. Most lipid and lipoprotein risk markers improved or were unaffected; an undesirable change was observed in one marker.¹

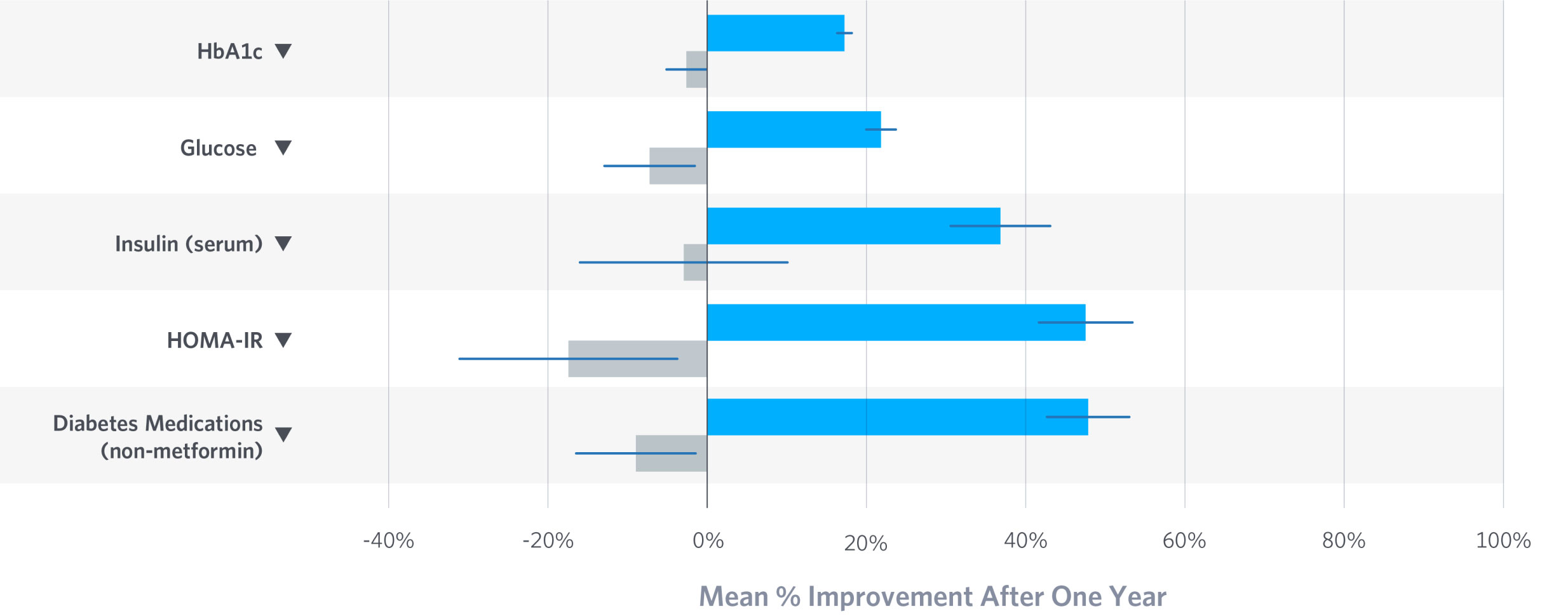
Type 2 Diabetes
While reducing and eliminating glycemic control medications, Virta patients lowered HbA1c by 1.3% on average after one year and improved insulin resistance measured by HOMA-IR. 60% of patients enrolled one year attained an HbA1c below 6.5% without the use of diabetes medications other than metformin.

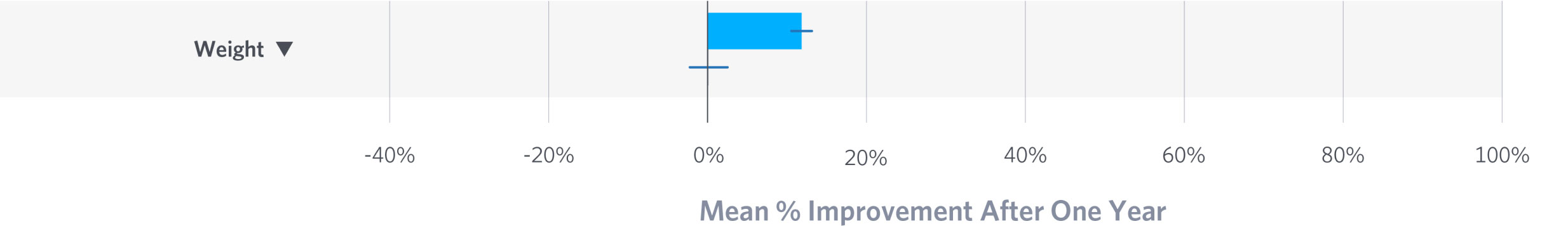
Obesity
Excess weight represents risk for both type 2 diabetes and cardiovascular disease. Virta patients sustained the loss of 12% of their body weight over the year. The prevalence of class III obesity among participants was reduced from 46% to 20%.

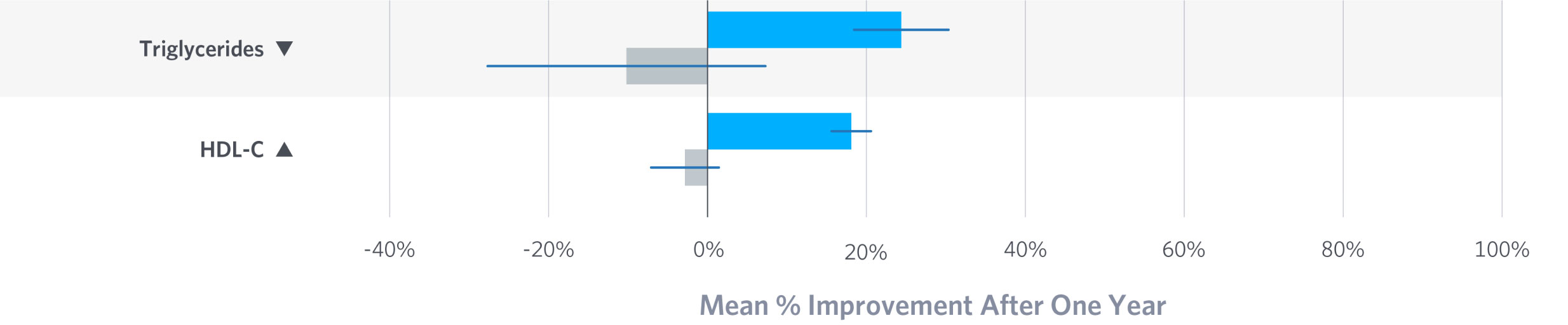
Atherogenic Dyslipidemia
Characterized by high triglycerides and low HDL-C, atherogenic dyslipidemia is common among patients with insulin resistance and represents increased cardiovascular risk. Virta patients improved both markers, with the TG/HDL-C ratio declining from 4.7 to 3 on average.

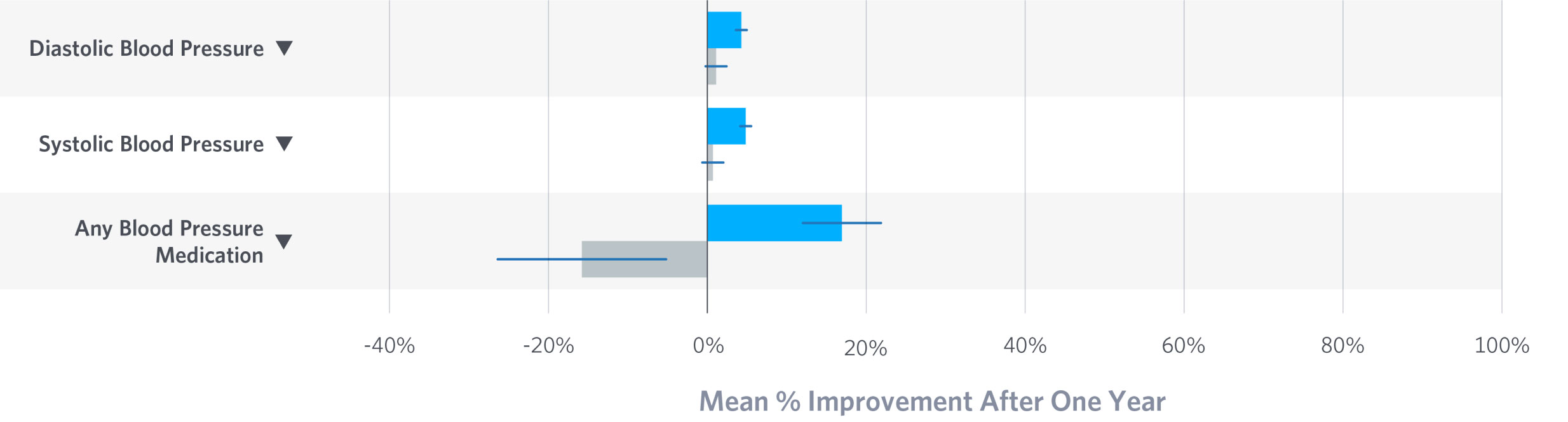
Hypertension
Elevated blood pressure, especially in the presence of additional risk factors, increases cardiovascular risk. Virta patients reduced blood pressure and the need for antihypertensive medication, especially diuretics.

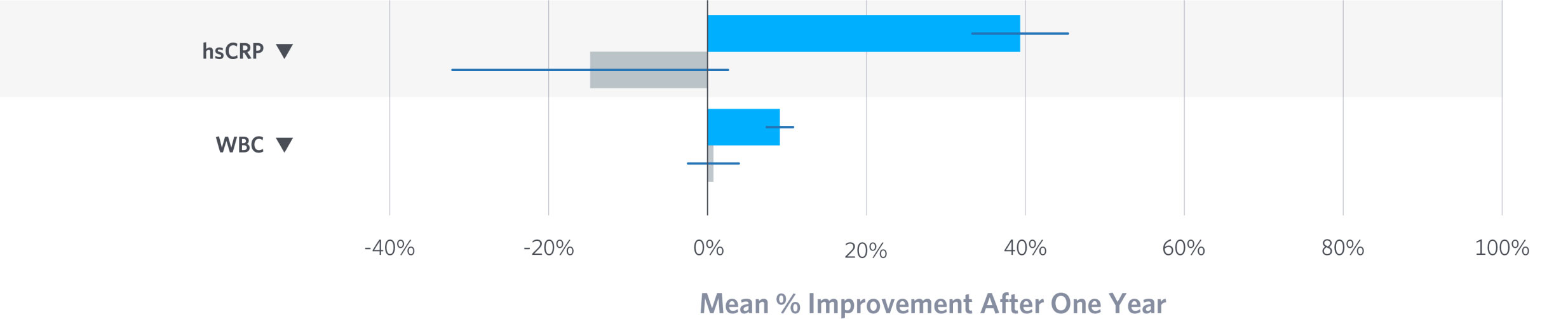
Inflammation
Inflammation is a common underlying factor in obesity, insulin resistance, hypertension, and cardiovascular disease. C-reactive protein and white blood cell count, common markers of inflammation, were significantly reduced in Virta patients with type 2 diabetes.

Safety
A common concern in the treatment of type 2 diabetes is hypoglycemia. In our clinical trial, no hypoglycemic events requiring assistance were reported. Additionally, treatment at Virta resulted in neutral or positive effects on markers of kidney and liver function.

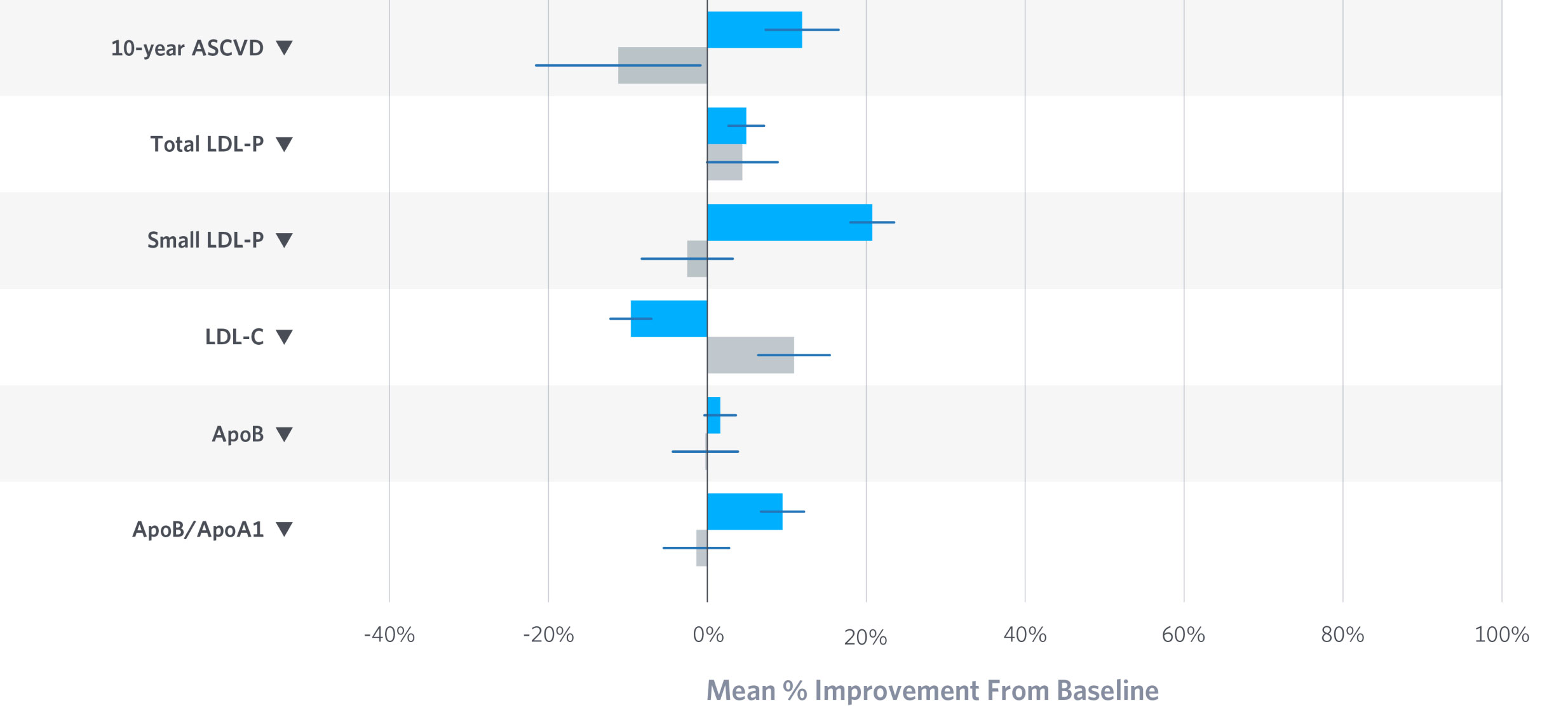
Cardiovascular Risk Markers
10-year ASCVD risk score improves after one year of the Virta Treatment. Most lipid and lipoprotein risk markers improved or were unaffected; an undesirable change was observed in one marker.

Publications
Peer-reviewed papers

Long-term, sustainable benefit to key diabetes outcomes
At two years of treatment, Virta trial patients still experienced clinically significant improvements in HbA1c %, metabolic syndrome rate, and markers of inflammation. More than half of trial completers met the criteria for diabetes reversal, and a significant portion of those individuals also had partial and complete diabetes remission. Along with these improvements in health outcomes, 67% of diabetes-specific prescriptions were discontinued, and 91% of patients who began on insulin either reduced or eliminated their insulin dosage.

Continued improvement in health outcomes at 1 year
After one year of treatment, patients who chose Virta improved glycemic control and markers of other chronic conditions. 94% of patients on insulin reduced or eliminated their dosage. Average weight loss was 12%. Other improvements included markers of cardiovascular disease, inflammation, and liver function.

Rapid impact on type 2 diabetes
The first investigation of Virta’s novel care model demonstrated that patients could rapidly improve glycemic control through reductions in fasting blood glucose, HbA1c, and medication use after 10 weeks of treatment. Patients lost 7% of their body weight on average and reported less hunger.

Long-term prediabetes reversal and type 2 diabetes prevention
Virta studied the effects of its intervention in patients with prediabetes and found that only 3% of trial participants progressed to type 2 diabetes over a two year period. Over half of participants achieved normoglycemia, with 75% of patients retained at the two-year mark.

Long-term improvement in cardiovascular risk factors
Virta examined markers of cardiovascular disease at two-years and found that patients living with type 2 diabetes sustained improvements in multiple cardiovascular risk factors. This includes long-term improvement in traditional markers of atherogenic dyslipidemia (triglycerides and HDL cholesterol) and a substantial reduction in pro-atherogenic small LDL particles.
Significant impact on cardiovascular risk factors
For patients living with type 2 diabetes, the risk of cardiovascular disease (CVD) is higher than average and CVD is the leading cause of mortality. There is a need for interventions that mitigate cardiovascular risk in addition to improving glycemic control and markers of insulin resistance. On average, the Virta Treatment improved or had no effect on most markers of cardiovascular risk. For the subset of individuals whose key markers did not improve, the range of responses were similar to those observed in participants who pursued the usual care for their type 2 diabetes.

Sustained improvement in depressive symptoms at 2 years
Virta patients experienced rapid and sustained improvement in depressive symptoms, with nearly one-third fewer patients meeting the clinical cutoff for depression at two years. Depressed patients followed a similar pattern of metabolic health improvement compared to those without a past diagnosis.

Evidence of non-alcoholic fatty liver disease improvement
An estimated 60% of American adults living with type 2 diabetes have non-alcoholic fatty liver disease (NAFLD), and the only treatment currently endorsed by professional guidelines for NAFLD is weight loss. At one year, almost 80% of patients with type 2 diabetes who participated in the Virta treatment lost more than 5% of their starting body weight, which is associated with improvement in steatosis. Concurrent with 12% average weight loss, liver enzyme concentrations, surrogate scores for liver steatosis and fibrosis, and inflammation improved in these patients.

Long-term improvement in knee pain and function
Osteoarthritis (OA) is a painful and debilitating condition affecting more than 54 million U.S. adults (nearly 23%) annually. Among adults with diabetes, the prevalence of OA increases to an estimated 48.1%. Virta patients with type 2 diabetes, however, experienced significant long-term improvement in knee pain and function from baseline to two years.
Advancing science and medicine

- Hallberg SJ et al. Diabetes Therapy. 2018;9(2):583-612 and Bhanpuri NH et al. Cardiovasc Diabetol. 2018; 17:56.


























