To Reverse Type 2 Diabetes, Flip the Food Pyramid Upside Down

“Type 2 diabetes is a chronic and progressive disease,” I used to tell my Type 2 diabetes patients. The best I could do was encourage them to eat right and to exercise, while adding more and more prescriptions over the years.
My entire view on type 2 diabetes has shifted. I’ve spent the last few years helping patients reverse their diabetes, regain energy, and feel better. Taking my patients off of their medications feels really good. To reverse type 2 diabetes safely and sustainably, we need to flip the food pyramid upside down, prescribing patients with type 2 diabetes a low carb, high fat diet administered under medical supervision.
A low carb, high fat diet puts patients into nutritional ketosis, a metabolic state of burning fat and using ketones rather than glucose for energy. Nutritional ketosis is clinically proven to directly reduce blood glucose (as measured by A1C and blood glucose readings), improve insulin sensitivity (as measured by HOMA-IR), and reduce inflammation (as measured by CRP). A clinical trial showed that with nutritional ketosis, health coaching, and medical supervision, 56% of patients were able to lower their HbA1c below the diagnostic threshold for type 2 diabetes in 10 weeks. 87% of patients who began the clinical trial on insulin were able to reduce or eliminate insulin entirely.¹
I’m saying “reversed” rather than “cured” because type 2 diabetes is reversible but it may resurface without maintenance. Nutritional ketosis, bariatric surgery, and hypocaloric diets show clinical evidence of diabetes reversal, including reduced or eliminated diabetes medications. However, nutritional ketosis is the most effective treatment for sustainably reversing type 2 diabetes because patients can stick with it. At six months, 89% of patients in the aforementioned clinical trial were still enrolled and adhering to the protocol.²
Nutritional ketosis as a tool to reverse type 2 diabetes: How does it work?
Type 2 diabetes is characterized by high blood glucose. Carbohydrate consumption elevates patients’ blood glucose more than protein or fat do, but unlike carbs and protein, fat isn’t converted into glucose. Furthermore, fat doesn’t require insulin to convert into energy, so it bypasses insulin resistance.
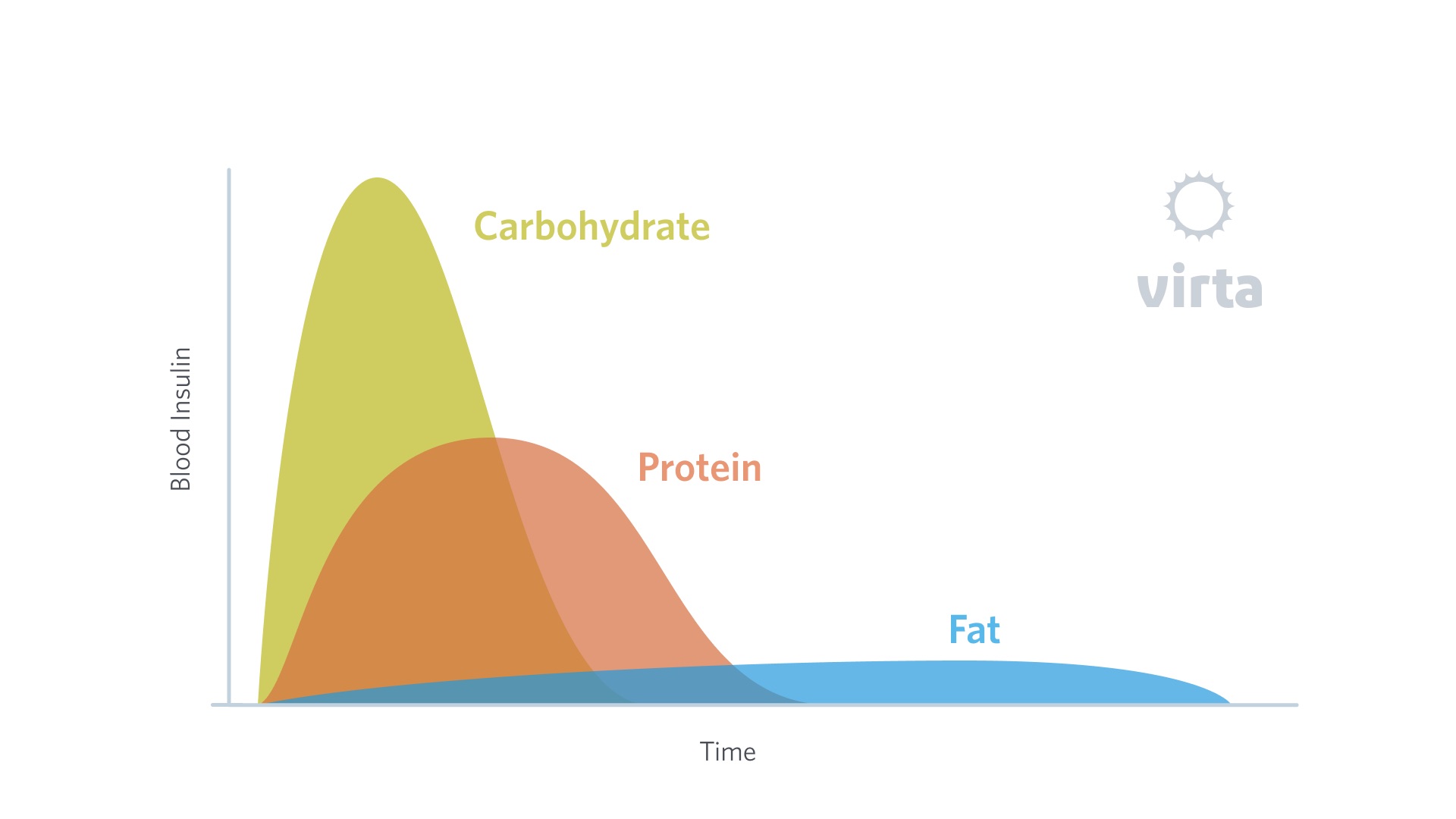
When a non-diabetic person eats a cup of brown rice (about 45 grams of carbs, which becomes nine teaspoons of glucose in the blood), blood glucose rises, which triggers beta cell insulin secretion. Rising circulating insulin drives glucose into cells, and the blood glucose remains in the normal range. In type 2 diabetes, insulin resistance interrupts this process, and both insulin and blood glucose remain high. In this sense, we can reframe insulin resistance as carbohydrate intolerance. While adding injected insulin can lower blood glucose in the short term, it doesn’t resolve the underlying problem of insulin resistance.
Will increased fat consumption lead to high cholesterol?
Contrary to national dietary guidelines, a high fat diet is clinically effective for weight loss if carbohydrates are restricted and protein is moderated. The dominating theory that dietary fat causes heart disease and high cholesterol has been largely debunked.³⁻⁸
What is the timeline for nutritional ketosis to reverse diabetes?
In nutritional ketosis, fasting and meal-time blood glucose rapidly decrease within a few weeks. In three-to-four months, the A1c has improved or even normalized. Sustained nutritional ketosis can lead to maintenance of normal blood glucose even with the removal of most or all diabetes medications.
Not all diets are created equal but a well-formulated ketogenic diet, based on whole foods, is a healthy and sustainable way to reverse type 2 diabetes. Reduction of medications under medical supervision allows people with Type 2 diabetes to safely return to a normal metabolic state.
This blog is intended for informational purposes only and is not meant to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition or any advice relating to your health. View full disclaimer
Are you living with type 2 diabetes, prediabetes, or unwanted weight?

- McKenzie AL, Hallberg SJ, Creighton BC, Volk BM, Link TM, Abner MK, Glon RM, McCarter JP, Volek JS, Phinney SD. Novel Intervention including Individualized Nutritional Recommendations Reduces HbA1c, Medication Use, and Weight in Type-2 Diabetes. JMIR Diabetes. 2017; 2(1):e5. doi: 10.2196/diabetes.6981
- McKenzie A, Bhanpuri N, McCarter J. Clinical Trial Update: 6 month outcomes in patients with type 2 diabetes [white paper]. 2017. Virta Health. Retrieved from http://assets.virtahealth.com/docs/Virta_Clinic_6-month_outcomes.pdf
- Dehghan M, Mente A, Zhang X, et al. Associations of fats and carbohydrate intake with cardiovascular disease and mortality in 18 countries from five continents (PURE): a prospective cohort study. Lancet. 2017 Aug 28. pii: S0140-6736(17)32252-3. doi: 10.1016/S0140-6736(17)32252-3.
- Ravichandran M, Grandl G, Ristow M. Dietary Carbohydrates Impair Healthspan and Promote Mortality. Cell Metab. 2017; 26:585-587. doi: 10.1016/j.cmet.2017.09.011. 85 - 587.
- National Academies of Sciences, Engineering, and Medicine. 2017. Redesigning the Process for Establishing the Dietary Guidelines for Americans. Washington, DC: The National Academies Press. https://doi.org/10.17226/24883.
- Seshadri P, Iqbal N, Stern L, Williams M, Chicano KL, Daily DA, McGrory J, Gracely EJ, Rader DJ, Samaha FF. A randomized study comparing the effects of a low-carbohydrate diet and a conventional diet on lipoprotein subfractions and C-reactive protein levels in patients with severe obesity. Am J Med. 2004; 117:398-405.
- Shai I, Schwarzfuchs D, Henkin Y, Shahar DR, Witkow S, Greenberg I, Golan R, Fraser D, Bolotin A, Vardi H, Tangi-Rozental O, Zuk-Ramot R, Sarusi B, Brickner D, Schwartz Z, Sheiner E, Marko R, Katorza E, Thiery J, Fiedler GM, Blüher M, Stumvoll M, Stampfer MJ. Weight loss with a low-carbohydrate, Mediterranean, or low-fat diet Dietary Intervention Randomized Controlled Trial (DIRECT) Group. N Engl J Med. 2008; 359:229-41.
- Hays JH, DiSabatino A, Gorman RT, Vincent S, Stillabower ME. Effect of a high saturated fat and no-starch diet on serum lipid subfractions in patients with documented atherosclerotic cardiovascular disease. Mayo Clin Proc. 2003; 78:1331-6.